How to Treat and Prevent Shin Splints: A Complete Recovery Guide

This article is for general educational purposes only and does not constitute medical or professional fitness advice.
Consult a licensed healthcare provider before starting any new exercise program, especially if you have a pre-existing condition.
Shin splints are among the most common running-related injuries — particularly for beginners who increase their mileage too quickly.
The good news: most cases are manageable with conservative approaches and respond well to load modification, specific exercises, and patience.
This guide covers the causes, a step-by-step recovery framework, and evidence-informed prevention strategies.
What Are Shin Splints? Causes and Anatomy
The Clinical Term
The clinical term for shin splints is Medial Tibial Stress Syndrome (MTSS) — a stress response of the tibia (the larger of the two lower leg bones, running from the knee to the ankle) and the surrounding connective tissue to repetitive mechanical loading.
Pain is typically felt along the inner border of the shinbone during and after exercise, and in early stages often diminishes within the first few minutes of activity before returning.
Common Contributing Factors
| Factor | How It Contributes |
|---|---|
| Rapid training load increase | Bone and connective tissue adapt more slowly than muscle — outpacing adaptation is the most common cause |
| Hard or unforgiving surfaces | Concrete transmits higher peak impact forces than grass, track, or treadmill surfaces |
| Worn-out footwear | Midsole cushioning degrades after 500–700 km — increasing impact transmission |
| Weak hip abductors or glutes | Can cause excessive tibial rotation under load |
| Overpronation | Excessive inward rolling of the foot increases medial tibial stress with each stride |
When to Seek Medical Evaluation
• Pain is focal (a single sharp spot) rather than diffuse along the shin — this may indicate a stress fracture, which requires imaging to rule out
• Pain is present at rest or wakes you from sleep
• The shin is visibly swollen, warm, or bruised
• Symptoms do not improve with 2–3 weeks of load reduction
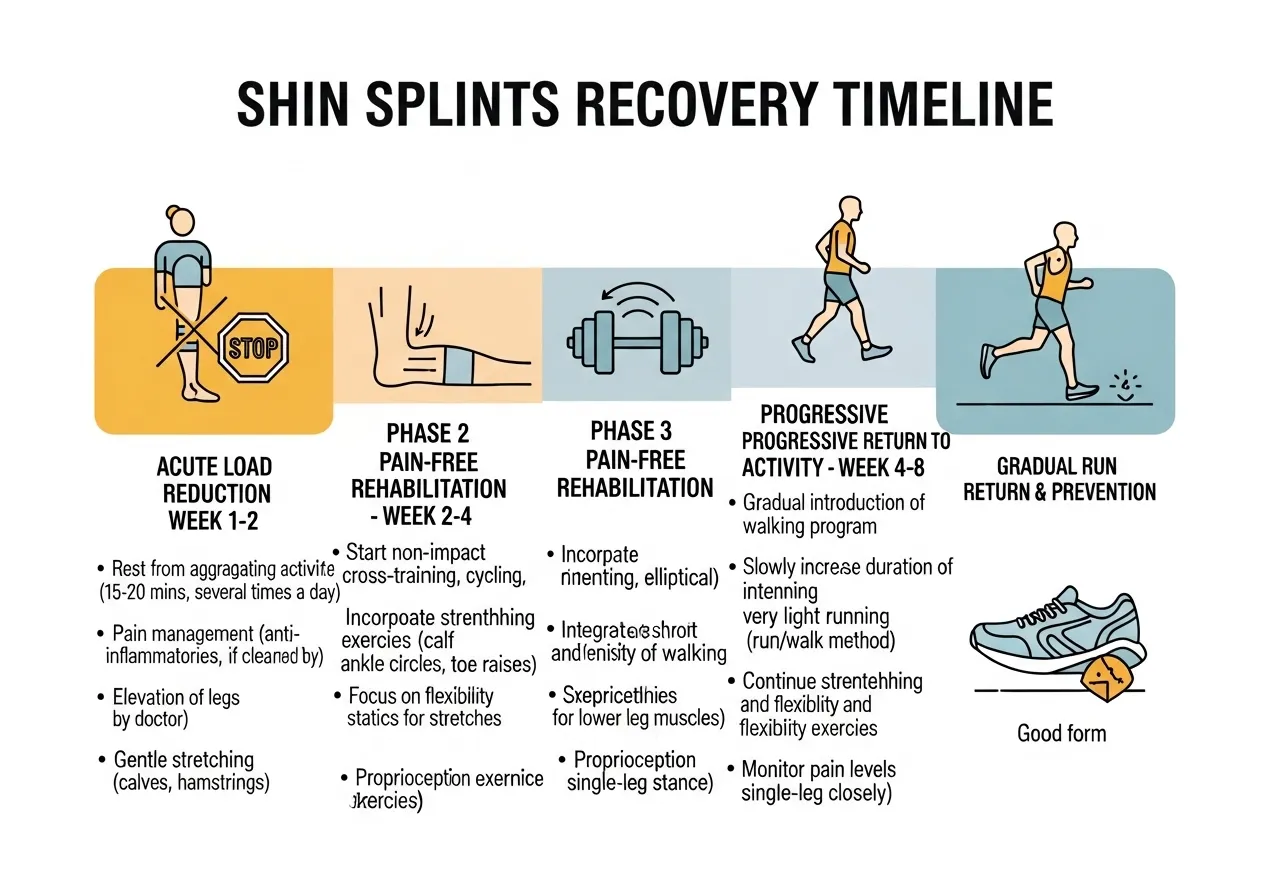
The 4-Phase Recovery Framework
Phase 1 — Load Reduction (Days 1–7)
The primary goal in the acute phase is to reduce the tibial stress that is driving the inflammatory response — without complete inactivity if avoidable.
✅ Replace running sessions with lower-impact alternatives: swimming, cycling, pool running (aqua jogging — running motion in deep water, which maintains cardiovascular fitness with near-zero tibial impact)
✅ Ice the affected area for 10–15 minutes after activity if helpful for symptom management
✅ Avoid activities that reproduce or significantly worsen the pain
Phase 2 — Rehabilitation Exercises (Weeks 1–3)
Strengthening the muscles that support the tibia during running reduces the stress placed on the bone and surrounding tissue:
✅ Tibialis anterior raises (flexing the foot upward against resistance): 3 × 15
✅ Single-leg balance: 3 × 30 sec, progressing to unstable surface
✅ Hip strengthening: clamshells, glute bridges — 3 × 15 each
Phase 3 — Gradual Return to Running (Weeks 3–6)
Return to running using a run-walk protocol — alternating periods of running and walking to gradually reload the tibia:
Week 4: 2 min run / 1 min walk × 8 rounds
Week 5: 5 min run / 1 min walk × 5 rounds
Week 6: 10–15 min continuous easy run (if pain-free throughout)
Phase 4 — Full Return and Prevention (Week 6+)
Once continuous running is pain-free, focus on prevention strategies outlined in the next section.
Maintaining the strengthening exercises 2×/week long-term is generally recommended — not just during active recovery.

7 Evidence-Aligned Prevention Strategies
1 — Follow the 10% Rule
Increasing weekly running volume by no more than approximately 10% per week is a widely cited guideline for managing tibial bone stress accumulation.
Bone remodeling takes 6–8 weeks to meaningfully adapt to new loading — faster progression may outpace this adaptive capacity.
2 — Replace Footwear Regularly
Running shoe midsoles typically lose meaningful cushioning after 500–700 km of use — even when the upper looks fine externally.
If you have been wearing the same shoes for over 6–9 months with regular running, evaluating their cushioning (try pressing a thumbnail firmly into the midsole — significant compression resistance should be present) may be worthwhile.
3 — Vary Your Running Surface
Concrete produces higher peak tibial forces than softer surfaces. Incorporating grass, dirt trails, or track running into your weekly mix may reduce cumulative tibial stress over time.
4 — Strengthen the Lower Leg and Hip Complex
Consistent calf strengthening (including the soleus, which absorbs significant force during running), tibialis anterior work, and hip abductor exercises may reduce the mechanical factors that contribute to MTSS recurrence.
5 — Address Overpronation if Present
Significant overpronation (excessive inward rolling of the foot after heel strike) can be addressed through motion-control or stability footwear, custom orthotics, or specific foot strengthening work.
A podiatrist or sports medicine physician can assess whether overpronation is clinically relevant in your case.
6 — Include Rest Days
Bone remodeling requires rest — it does not happen during the run itself, but in the recovery periods between runs.
Running every single day without adequate recovery days between sessions significantly increases MTSS risk, particularly in beginners.
7 — Warm Up Before Running
A brief dynamic warm-up (5–8 minutes of walking, leg swings, ankle circles, and heel-to-toe walks) before running increases circulation to the lower leg and prepares the tibial stress response mechanism before impact loading begins.

Frequently Asked Questions About Shin Splints
Q: Can I run through shin splints?
This depends on severity. Mild discomfort that warms up within a few minutes and does not worsen during or after the run may be manageable with reduced intensity.
Running through moderate-to-severe pain risks progressing MTSS into a tibial stress fracture (a more serious injury involving an actual crack in the bone) — which requires complete rest from impact activities for 6–8 weeks or more.
When in doubt, please consult a sports medicine physician or physical therapist before continuing to run with shin pain.
Q: How long does recovery typically take?
Mild MTSS often improves within 2–6 weeks of appropriate load reduction and rehabilitation.
More significant cases may require 8–12 weeks of graduated recovery before returning to pre-injury mileage.
Repeatedly pushing through pain and skipping rehabilitation tends to extend the total recovery timeline significantly — patience in the early stages generally leads to faster overall return to full training.
Q: Are shin splints the same as a stress fracture?
No — they are related but different conditions on a continuum of tibial bone stress.
MTSS involves diffuse pain and a stress reaction in the bone and connective tissue. A stress fracture involves an actual micro-crack in the cortical bone (the dense outer layer of the bone) and produces focal point tenderness — pain when pressing a specific small area of the shinbone.
Stress fractures require medical imaging to diagnose and typically need complete rest from impact for 6–8+ weeks. If pain is localized to a specific spot rather than diffuse along the shin, medical evaluation is strongly recommended.
- Shin splints most commonly result from training load increasing faster than bone adaptation can occur
- Focal point pain (one sharp spot) warrants medical imaging to rule out a stress fracture
- The 4-phase framework (load reduction → rehab exercises → run-walk return → prevention) is a practical recovery roadmap
- The 10% weekly mileage rule is a widely used preventive guideline
- Consult a sports medicine physician or physical therapist for any shin pain that does not improve within 2–3 weeks






